Gynaecology Ultrasound Guide
Pelvic | Adolescent pelvic | Deep Endometriosis | Complex gynae | Fertility | Follicle Tracking
We understand that having an ultrasound can feel daunting, especially when you are unsure of what to expect. At Central West Women's Imaging, your comfort and wellbeing are at the heart of everything we do. This guide has been prepared to help you feel informed, at ease, and confident before your appointment.
Our sonographers are specialists in obstetric and gynaecological ultrasound, with advanced training in areas including deep endometriosis imaging and 3D pelvic assessment. We use dedicated GE women's imaging ultrasound machines, recognised as some of the most advanced equipment available for women's health, to ensure we obtain the highest quality diagnostic images for you and your referring doctor.
Our Promise to You
• We take the time to listen and explain what we are seeing during your scan
• Your consent is central to every step of your examination
• Our ultrasound rooms are thoughtfully designed for your comfort and privacy
• We are committed to compassionate, expert care for women of all backgrounds
• If you have any concerns at all, please let us know — we are here for you
Use this guide to find information about your specific ultrasound appointment. Each section explains what the scan involves, what to expect on the day, and how to prepare.
Further Information

What is a pelvic ultrasound?
1
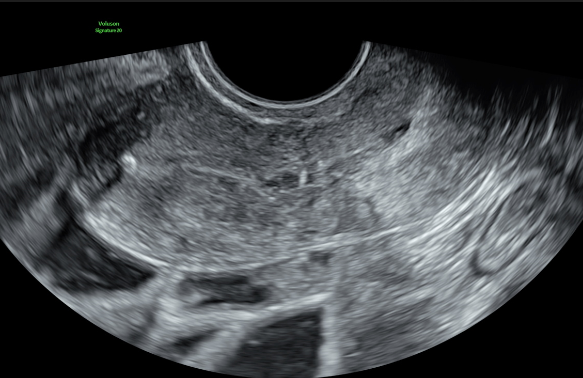
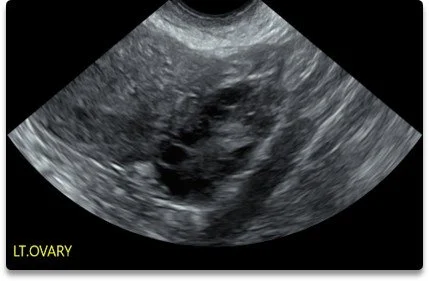
A pelvic ultrasound is a detailed assessment of your uterus, ovaries, and surrounding pelvic structures using sound waves. It is one of the most informative investigations available for gynaecological concerns and is completely safe — there is no radiation involved.
Why might your doctor refer you for a pelvic ultrasound?
Irregular, heavy, or prolonged periods
Pelvic pain (acute or chronic)
Investigation of ovarian cysts, fibroids, or polyps
Assessment of the uterine lining (endometrium)
Polycystic ovary syndrome (PCOS) screening
Post-menopausal bleeding
Assessment of the position of an intrauterine device (IUD)
General gynaecological check-up
What happens during your scan?
2
Part 1: Transabdominal Assessment
Your examination begins with a transabdominal scan. Your sonographer will apply a small amount of warm gel to your lower abdomen and gently move an ultrasound transducer across the area. Looking through your comfortably full bladder, we are able to see your uterus, ovaries, and surrounding structures. This part of the scan is performed over your clothing-free abdomen and is painless.
Part 2: Transvaginal Assessment
This is performed with your consent. A transvaginal (internal) ultrasound provides much higher resolution, highly detailed images of your pelvic organs and is considered the gold standard for gynaecological imaging. If a transvaginal (internal) scan is recommended, we will explain why and answer any questions before proceeding.
➤ For more information about what a transvaginal ultrasound involves, please see our Transvaginal Ultrasound Information section at the end of this guide.
How to Prepare
• Timing: Where possible, the best time for a routine pelvic ultrasound is between days 5 and 10 of your menstrual cycle (day 1 being the first day of your period), unless your doctor has advised otherwise, or you do not have a regular cycle.
• Bladder: Please arrive with a comfortably full bladder. We suggest drinking approximately 300 ml of water about one hour before your appointment and avoiding emptying your bladder until after the transabdominal portion of your scan.
• Clothing: Wear comfortable, loose-fitting clothing for easy access to your lower abdomen.
• Appointment length: Approximately 30 minutes.
• What to bring: Your referral letter and Medicare card.
What is an adolescent pelvic ultrasound?
1
An adolescent pelvic ultrasound is a gentle, non-invasive assessment designed specifically for younger patients. Pelvic pain and menstrual concerns are common in adolescents and can be caused by a range of conditions. Ultrasound is the ideal first-line investigation because it is safe, uses no radiation, and can provide valuable diagnostic information without discomfort.
We understand that this can feel particularly daunting for younger patients. Our sonographers are experienced in working with adolescents and their families, and we take extra time to explain each step in an age-appropriate and reassuring way. A parent or guardian is welcome to be present throughout the scan.
Why might your doctor refer a young person for a pelvic ultrasound?
2
Common reasons for referral in adolescents include:
Painful periods (dysmenorrhoea) or chronic pelvic pain
Heavy or irregular menstrual bleeding
Absence of periods (primary amenorrhoea)
Investigation of ovarian cysts or adnexal masses
Assessment for reproductive tract anomalies (such as uterine abnormalities or obstructive conditions)
Screening for polycystic ovary syndrome (PCOS)
Unexplained acute pelvic or abdominal pain (including concerns about ovarian torsion)
Endometriosis is increasingly recognised in adolescents and is often underdiagnosed in younger patients. If your doctor suspects endometriosis, a specialised endometriosis ultrasound may be recommended.
What happens during your scan?
3
For adolescent patients, the scan is typically performed transabdominally only — through the lower abdomen using a gentle external probe. A small amount of warm gel is applied and the sonographer moves the transducer across the skin to obtain images of the uterus and ovaries. A comfortably full bladder helps provide clear images.
A transvaginal scan is not routinely performed in adolescent patients. If a transvaginal assessment would provide important additional information and the patient is comfortable and willing, it may be discussed as an option, but it is never required and is always the patient's choice.
How to Prepare
• Bladder: Please arrive with a comfortably full bladder (approximately 500 ml of water one hour before the appointment).
• Clothing: Wear comfortable, loose-fitting clothing.
• Appointment length: Approximately 30 minutes.
• What to bring: Your referral letter and Medicare card. A parent or guardian is welcome to accompany you.
What is a 3D Pelvic Ultrasound?
1
While many people associate 3D ultrasound with pregnancy imaging, 3D technology is equally valuable in gynaecological assessment. A 3D pelvic ultrasound uses advanced imaging to create a detailed, three-dimensional view of your uterus and pelvic structures that cannot be obtained with standard 2D scanning alone.
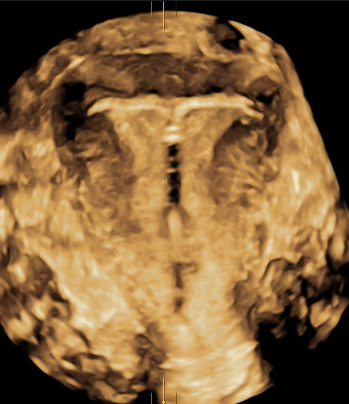
The most significant advantage of 3D ultrasound in gynaecology is the ability to visualise the coronal plane of the uterus — a view that shows the exact shape of the uterine cavity and its relationship to the surrounding muscle wall. This information was previously only available through MRI.
When is 3D ultrasound used?
2
Your sonographer may use 3D imaging as part of your pelvic assessment to:
Assess the shape of the uterine cavity (important for fertility investigations, recurrent miscarriage, and family planning)
Detect uterine anomalies such as a septate, bicornuate, or arcuate uterus
Evaluate polyps and submucosal fibroids within the uterine cavity
Confirm the position of an intrauterine device (IUD or Mirena)
Provide detailed assessment as part of a baseline fertility scan
3D imaging is integrated into our standard scanning protocol where clinically indicated. There is no additional discomfort — the 3D images are acquired during the same scan using our advanced GE ultrasound equipment.
➤ For more information about what a transvaginal ultrasound involves, please see our Transvaginal Ultrasound Information section at the end of this guide.
How to Prepare
• Bladder: Please arrive with a comfortably full bladder (approximately 500 ml of water one hour before the appointment).
• Clothing: Wear comfortable, loose-fitting clothing.
• Appointment length: Approximately 30 minutes.
• What to bring: Your referral letter and Medicare card. A parent or guardian is welcome to accompany you.
What is a Endometriosis?
1
Endometriosis is a condition where tissue similar to the lining of the uterus (endometrium) grows in other areas of the body, most commonly within the pelvis. It can cause significant pain, heavy periods, and difficulties with fertility. Endometriosis affects approximately one in ten women and people assigned female at birth (ASA Endometriosis Guidelines 2026).
What are the subtypes of endometriosis?
2
According to the ASA Endometriosis Guidelines (2026), endometriosis is classified into four subtypes based on lesion location and depth. These may occur independently or in combination, and accurate classification is essential for guiding diagnosis, treatment planning, and surgical approach:
Superficial peritoneal disease — Lesions confined to the surface of the peritoneum, typically affecting pelvic and abdominal viscera. These small lesions have no significant mass and are rarely seen on ultrasound; they are most reliably identified during laparoscopy (keyhole surgery).
Ovarian endometriomas — Cystic lesions within the ovaries, commonly referred to as “chocolate cysts” due to their appearance at surgery. These are readily identified on ultrasound.
Deep endometriosis — The most clinically significant subtype, often associated with severe symptoms and complex surgical management. Deep endometriosis involves endometrial-like tissue infiltrating on or beneath the peritoneum, commonly affecting the uterosacral ligaments, bladder, bowel, pelvic wall, and retroperitoneal spaces. Because these lesions have enough mass to distort anatomy, they can be detected by a specialised ultrasound performed by an appropriately trained sonographer.
Extra-pelvic endometriosis — Lesions located outside the pelvic cavity, including the appendix, diaphragm, abdominal wall, thoracic cavity, and, in rare cases, the brain.
An important note: An ultrasound cannot completely rule out endometriosis, because superficial disease is not always visible on ultrasound. A laparoscopy may still be recommended if symptoms are significant and the ultrasound appears normal. However, when deep endometriosis is identified on ultrasound, this allows your surgeon to plan the most appropriate procedure and reduces the chance of needing a second operation.
How to Prepare
• Timing: If you have periods, days 5 to 10 of your cycle is ideal, unless otherwise directed by your doctor. If you are on medication that stops your periods, any time is fine.
• Bladder: No full bladder is required for this scan. Please empty your bladder before the examination for your comfort.
• Bowel preparation: No specific bowel preparation is required. However, having a bowel motion on the morning of your scan can improve visualisation of deeper structures.
• Appointment length: Approximately 45 minutes.
• What to bring: Your referral letter, Medicare card, and any previous imaging reports or surgical notes if available.
What is a deep endometriosis ultrasound?
3
A deep endometriosis ultrasound is a specialised pelvic ultrasound designed to look for signs of deep endometriosis, this is not a standard pelvic ultrasound, although it feels just the same. The ASA Endometriosis Guidelines (2026) identify transvaginal (internal) ultrasound as the preferred first-line imaging modality for evaluating gynaecological symptoms, including suspected endometriosis, and recommend it for identifying the origin of symptoms, mapping disease, and assessing the extent of lesions to support both surgical planning and patient counselling.
At Central West Women's Imaging, our sonographers are clinical experts in this area. They have completed tertiary-level training in deep endometriosis imaging and continue to upskill through ongoing professional development and research involvement. We follow a systematic, evidence-based approach aligned with the ASA Endometriosis Guidelines (2026) to carefully assess each area where endometriosis is commonly found.
What does the scan assess?
4
During your endometriosis ultrasound, our clinical experts methodically evaluate a number of structures beyond the standard pelvic assessment, including:
The uterus (including assessment of adenomyosis)
Both ovaries (including screening for endometriomas)
The vaginal walls and underlying fascia
The uterosacral ligaments
The parametrium (the supporting tissue beside the uterus)
The vesico-uterine pouch (between the bladder and uterus)
The retrovaginal septum and retrovaginal space (also known as the pouch of Douglas)
The bladder wall
The ureters (the tubes from the kidneys to the bladder) and kidneys
The bowel wall (of the lower segment)
What happens during the scan?
5
The endometriosis ultrasound is performed as a transvaginal (internal) scan. The transvaginal approach is essential for this assessment, as it allows us to see the deeper structures of the pelvis in fine detail. Your sonographer may apply gentle pressure with the transvaginal transducer and use specific techniques such as the “sliding sign” to assess whether organs are moving freely or if adhesions may be present.
While some women experience mild tenderness during certain parts of this assessment, we will always communicate what we are doing and check in with you throughout. At the conclusion of your scan, your sonographer will take the time to discuss the findings with you and explain what has been seen. A detailed report and images will also be sent to your referring doctor.
➤ For more information about what a transvaginal ultrasound involves, please see our Transvaginal Ultrasound Information section at the end of this guide.
What is a Baseline Fertility ultrasound?
1
A baseline fertility ultrasound is a detailed pelvic assessment tailored specifically to evaluate your reproductive health when you are planning a pregnancy or experiencing difficulties conceiving. It provides your fertility specialist or GP with important baseline information to help guide your care.
Two of the most important components of this scan are the antral follicle count and 3D assessment of the uterine cavity. Together, these provide critical information about your ovarian reserve and the suitability of the uterine environment for pregnancy.
What does the scan assess?
2
Antral Follicle Count (AFC)
This is a count of the small resting follicles visible on each ovary. The AFC is one of the most reliable ultrasound markers of ovarian reserve — the number of eggs remaining in the ovaries. This information, often combined with blood tests such as AMH (anti-Müllerian hormone), helps your fertility specialist understand your reproductive potential and plan the most appropriate treatment.
3D Uterine Cavity Assessment
Using advanced 3D ultrasound imaging and reconstruction, we obtain a detailed coronal view of your uterine cavity. This allows us to accurately assess the cavity shape, identify any uterine anomalies (such as a septate or bicornuate uterus), and detect polyps or submucosal fibroids that may affect implantation. This level of detail was previously only available through MRI.
Additional Assessments
Ovarian volume: the size of each ovary, which can indicate conditions such as polycystic ovary syndrome
Endometrial lining: assessment of the thickness and pattern of the uterine lining
General pelvic survey: assessment of surrounding pelvic structures
➤ For more information about what a transvaginal ultrasound involves, please see our Transvaginal Ultrasound Information section at the end of this guide.
How to Prepare
• Timing: Your fertility team will advise the optimal timing for your baseline fertility assessment based on your treatment plan.
• Bladder: No full bladder is required. Please empty your bladder before the examination for your comfort, as the assessment is performed transvaginally.
• Appointment length: Approximately 30 minutes.
• What to bring: Your referral letter, Medicare card, and any blood test results or previous imaging your doctor has requested us to review.
What is a follicle tracking?
1
If you are undergoing ovulation induction, timed intercourse cycles, or assisted reproductive treatment (such as IUI or IVF), you may require follicle tracking ultrasounds. These are shorter, focused scans performed at specific points in your cycle to monitor the growth and development of your ovarian follicles and the thickness of your endometrial lining.
Follicle tracking provides your fertility specialist with real-time information about how your ovaries are responding to treatment, helping to determine the best timing for procedures such as insemination, egg collection, or intercourse.
What happens during the scan?
2
Follicle tracking is performed as a transvaginal ultrasound. The scan measures the size of the developing follicles on each ovary and assesses the endometrial lining. It is a quick and focused assessment. Your sonographer will communicate the results to your fertility clinic promptly so that your treatment can be adjusted as needed.
➤ For more information about what a transvaginal ultrasound involves, please see our Transvaginal Ultrasound Information section at the end of this guide.
How to Prepare
• Timing: Your fertility clinic will advise when to attend for each tracking scan, usually based on your treatment protocol.
• Bladder: No full bladder is required. Please empty your bladder before the scan for your comfort.
• Appointment length: Approximately 15 minutes.
• What to bring: Your referral letter.
What is a transvaginal ultrasound?
1
A transvaginal (internal) ultrasound is an internal scan that provides highly detailed images of your uterus, ovaries, and surrounding pelvic structures. Because the transducer is positioned close to the organs being assessed, it produces significantly higher resolution images than a transabdominal (external) scan. It is considered the gold standard for gynaecological imaging.
A transvaginal scan may be recommended as part of a pelvic ultrasound, endometriosis assessment, fertility scan, or follicle tracking appointment.
What happens during a transvaginal ultrasound?
2
You will be asked to empty your bladder before this part of the examination. When you return to the ultrasound room, a blanket will be provided for your privacy. You then remove your underwear and lie comfortably on the bed with your knees gently bent.
A slim, specially designed transducer — much narrower than a standard speculum — is covered with a sterile, single-use, latex-free protective sheath and a small amount of lubricating gel. The transducer is gently placed into the vagina. Some women prefer to insert this themselves, and that is completely up to you.
The transducer is moved gently from side to side to obtain detailed images. Your sonographer may lightly press on your lower abdomen with their other hand to move overlying bowel gas aside for clearer views. The length of the examination varies depending on the type of scan — your sonographer will explain what to expect on the day.
Most women find the transvaginal scan more comfortable than a Pap smear.
Is the transvaginal ultrasound compulsory?
3
No. The transvaginal component of any scan is only ever performed with your explicit consent. While it does provide significantly more detailed images of your pelvic organs, it is always your choice. If you prefer not to have a transvaginal scan, a transabdominal (external) ultrasound can be performed instead, although it may not provide the same level of detail. If you are unsure or nervous, please talk to us — we are here to support you and will never pressure you into any part of the examination.
You are in control at every stage of your scan.
Consent: We will always explain why a transvaginal scan is recommended and answer any questions before proceeding. You can ask us to stop at any time.
Probe covers: All our transvaginal probe covers are latex-free. We do not use latex anywhere in this examination. Please still let us know if you have any other allergies or concerns.
Virginity / no prior intercourse: A transvaginal ultrasound is generally not performed if you have not had sexual intercourse before. A transabdominal scan will be offered instead.
Support person: You are welcome to have a support person present during your scan if you wish.
Frequently Asked Questions
If you have any questions before your appointment, or would like to discuss any aspect of your scan, please do not hesitate to contact our friendly team.
-
Ultrasound is generally painless and safe. The transabdominal scan feels like gentle pressure on your abdomen. The transvaginal scan may feel slightly unusual, but most women find it more comfortable than a Pap test. For endometriosis assessments, some areas of tenderness may be encountered — your sonographer will always let you know what to expect and will check in with you throughout.
-
Standard pelvic ultrasound: approximately 30 minutes
Adolescent pelvic ultrasound: approximately 30 minutes
Deep endometriosis ultrasound: approximately 45 minutes
Baseline fertility assessment: approximately 30 minutes
Follicle tracking: approximately 15 minutes
-
Yes. You will need a current referral from your GP, gynaecologist, or fertility specialist to attend an ultrasound appointment. Please bring this with you on the day.
-
In most cases, we can still perform your ultrasound during your period. For some assessments (such as endometriosis), scanning during menstruation can actually provide helpful information. If you are unsure, please call us and we will advise whether to keep or reschedule your appointment.
-
Absolutely — we welcome you to bring one adult support person along. Please note that our waiting area and ultrasound room have limited space, so where possible we ask that children not attend the appointment. If you have any questions about this, feel free to email us at admin@cwwi.com.au before your visit.
-
Your detailed report and images are sent electronically to your referring doctor, usually within 24 to 48 hours. With your permission, we can also send you a link to images and short video clips from your scan that you can download and keep.
-
There is nothing special you need to do after your ultrasound — you can return to your normal activities straight away. There are no known side effects from diagnostic ultrasound.
-
Your reports and images are electronically sent to your referring doctor, giving them access to review the images as needed. We use a dedicated women's imaging reporting system and provide comprehensive reports prepared in collaboration with our specialist doctors, distributed to referrers via QUBS to ensure timely delivery.
