Obstetric Ultrasound Guide
Pregnancy Scans | Aneuploidy Screening | Fetal Wellbeing and Growth scans | 3D/4D Imaging
We understand that pregnancy is an exciting and sometimes anxious time. At Central West Women’s Imaging, your comfort and wellbeing are at the heart of everything we do. This guide has been prepared to help you feel informed, at ease, and confident before each of your pregnancy ultrasound appointments.
Our sonographers are specialists in obstetric and gynaecological ultrasound, with advanced training in fetal assessment, screening, and 3D/4D imaging. We use dedicated GE women’s imaging ultrasound machines, recognised as some of the most advanced equipment available for women’s health, to ensure we obtain the highest quality diagnostic images for you and your referring doctor.
Our Promise to You
• We take the time to listen and explain what we are seeing during your scan
• Your consent is central to every step of your examination
• Our ultrasound rooms are thoughtfully designed for your comfort and privacy
• We are committed to compassionate, expert care for women of all backgrounds
• If you have any concerns at all, please let us know — we are here for you
Use this guide to find information about your specific ultrasound appointment. Each section explains what the scan involves, what to expect on the day, and how to prepare.
Second Trimester
Multiple Pregnancies
Further Information
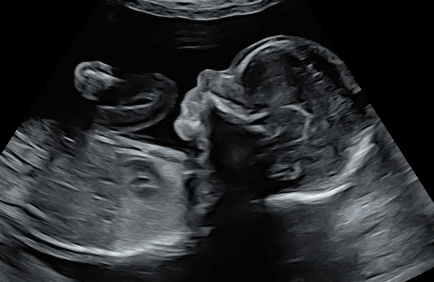
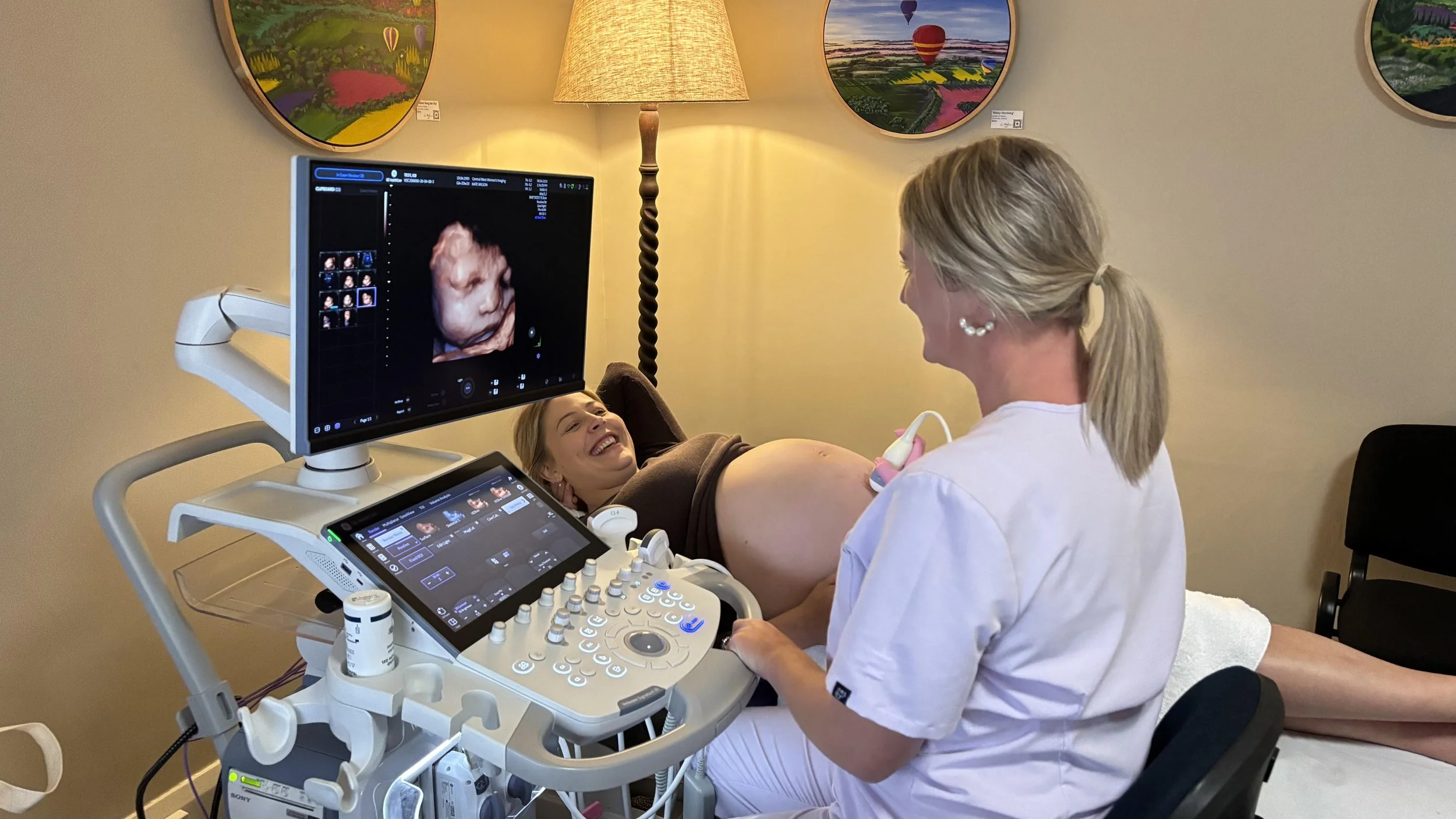
What is an ectopic pregnancy?
1
An ectopic pregnancy occurs when a fertilised egg implants outside the uterus, most commonly in one of the fallopian tubes. Ectopic pregnancies cannot continue to develop normally and require early detection and medical management to protect your health.
Warning signs to be aware of
2
If you experience any of the following symptoms in early pregnancy, please contact your doctor or present to your nearest emergency department promptly:
• Sharp or persistent pain on one side of your lower abdomen or pelvis
• Vaginal bleeding or spotting (which may differ from a normal period)
• Shoulder tip pain
• Dizziness, feeling faint, or generally feeling unwell
Early diagnosis significantly improves treatment options and outcomes.
How does ultrasound help?
3
Ultrasound is the primary tool used to assess the location of an early pregnancy. Your sonographer will look for a gestational sac within the uterus and carefully evaluate the fallopian tubes and surrounding structures. In some cases, an ectopic pregnancy can be directly identified on ultrasound; in other cases, the absence of an intrauterine pregnancy combined with your blood test results helps your doctor reach a diagnosis.
How to Prepare
• Timing: Your doctor will request this scan based on your symptoms and blood test results
• Bladder: Comfortably full bladder — 300 ml of water one hour before your appointment, and hold until your appointment
• Appointment length: Approximately 20–30 minutes
• What to bring: Your referral letter, Medicare card, and any recent blood test results
What to expect at your scan
4
Your appointment will include both a transabdominal and transvaginal (internal) ultrasound. The transvaginal (internal) component is particularly important in early pregnancy, as it provides significantly higher resolution images of the uterus and surrounding structures. A slim, sterile transducer is gently placed into the vagina, with your consent. Your sonographer will explain everything before and during the examination.
What is a dating scan?
1
A dating scan is usually the first ultrasound of your pregnancy. It is performed in the first trimester to confirm a viable intrauterine pregnancy, establish your expected due date, and determine whether you are carrying a single baby or multiples.
What does the scan assess?
2
• Confirmation that the pregnancy is located within the uterus
• Measurement of the embryo or fetus to establish gestational age and estimated due date
• Detection of a fetal heartbeat
• Number of babies (singleton or multiple pregnancy)
• Assessment of the uterus and ovaries
What to expect at your scan?
3
Your appointment will include both a transabdominal and transvaginal ultrasound. In very early pregnancy, the transvaginal component provides the most accurate images and measurements. Your sonographer will explain each step and ensure you are comfortable throughout.
How to Prepare
• Timing: Usually performed between 6 and 10 weeks of pregnancy, with 7–9 weeks being the ideal window
• Bladder: Comfortably full bladder — 300 ml of water one hour before your appointment, and hold until your scan is complete
• Appointment length: Approximately 20–30 minutes
• What to bring: Your referral letter and Medicare card
What is a Nuchal Translucency Screening?
1
The Nuchal Translucency (NT) screening, also known as the combined First Trimester Screening (cFTS), combines a detailed assessment of your baby’s anatomy, maternal blood tests and maternal risk factors. The detailed ultrasound includes a measurement of the thickness of the fluid at the back of the neck and the presence of the nasal bone. Together, these calculate the likelihood of chromosomal conditions including Down syndrome (Trisomy 21). Assessing your risk of developing pre-eclampsia later in pregnancy is performed in the same appointment by adding an ultrasound assessment of the blood flow through your uterine arteries and taking your blood pressure. Pre-eclampsia is a serious condition that affects approximately 2–5% of pregnancies in Australia.
What to expect at your scan
2
Your appointment is primarily transabdominal, although it may include transvaginal imaging. The NT measurement requires your baby to be in a specific position, so your sonographer may need a little extra time or ask you to move around gently to achieve the best images.
How to Prepare
• Timing: Between 11 weeks and 13 weeks + 6 days. We recommend between 12 weeks + 3 days and 13 weeks + 3 days for a detailed assessment of baby’s anatomy. We can arrange your appointment following a dating ultrasound once your due date is confirmed — contact us at admin@cwwi.com.au with any questions
• Bladder: Comfortably full bladder — 300 ml of water one hour before your appointment, and hold until your scan is complete
• Appointment length: Approximately 30–45 minutes
• What to bring: Your referral letter, Medicare card, and any blood test results your doctor has requested us to review
What is an early anatomy scan?
1
An early anatomy scan is a detailed assessment of your baby’s developing anatomy, performed earlier in pregnancy than the standard morphology scan. It provides an early opportunity to assess your baby’s brain, heart, spine, limbs, and other structures, and can help identify or exclude certain structural concerns sooner.
What does the scan assess?
2
• Baby’s brain and skull
• Heart and major blood vessels (early cardiac assessment)
• Spine
• Abdominal wall and organs
• Limbs, hands, and feet
• Placental position and amniotic fluid
Please note that an early structural check does not replace the morphology scan at 19–21 weeks, as some structures are better assessed later in pregnancy when they are more developed.
How to Prepare
• Timing: Usually between 14 and 17 weeks of pregnancy
• Bladder: Comfortably full bladder — 300 ml of water one hour before your appointment, and hold until your scan is complete
• Appointment length: Approximately 30 minutes
• What to bring: Your referral letter, Medicare card, and any previous imaging reports
What to expect at your scan?
3
Your appointment is primarily transabdominal, although it may include transvaginal imaging.
What is a morphology scan?
1
The morphology scan (also known as the anatomy scan or “20-week scan”) is one of the most important ultrasounds of your pregnancy. It is a comprehensive assessment of your baby’s anatomy, growth, and wellbeing, and provides your doctor with detailed information about your baby’s development.
What does the scan assess?
2
• Baby’s brain (neurology) and heart (fetal echocardiography), plus all other anatomy
• Baby’s size and measurements
• Placental position
• Cord insertion
• Cervical length (transvaginal measurement recommended)
How to Prepare
• Timing: Between 19 and 21 weeks of pregnancy (we do not accept bookings outside this window)
• Bladder: Please arrive with a comfortably full bladder — approximately 500 ml of water one hour before your appointment
• Appointment length: Approximately 45 minutes
• What to bring: Your referral letter, Medicare card, and any previous imaging reports
What to expect at your scan?
3
Your appointment is primarily transabdominal, although we recommend transvaginal imaging for the cervical length. Your sonographer will take the time to explain the findings and show you your baby during the examination.
What is a fetal growth and wellbeing scan?
1
A fetal growth scan monitors your baby’s size, growth pattern, and wellbeing in the third trimester. Your doctor may refer you for growth scans as part of routine third-trimester monitoring , if there are concerns about your baby’s growth or movements or if you have a medical condition such as gestational diabetes or high blood pressure.
What does the scan assess?
2
• Biometry measurements (Head Circumference, Abdominal Circumference, and Femur Length)
• Estimated Fetal Weight (EFW) and growth trajectory
• Amniotic fluid volume
• Doppler assessment including the umbilical artery, which assesses blood flow to your baby
• Placental position (see also Placenta Localisation below)
• Baby’s presentation and general wellbeing
How to Prepare
• Timing: As directed by your doctor (commonly from 28 weeks onwards, and may be repeated at intervals)
• Bladder: A comfortably full bladder is required until 34 weeks. After 34 weeks, there is no bladder preparation required
• Appointment length: Approximately 20–30 minutes
• What to bring: Your referral letter, Medicare card, and any previous growth scan reports
What to expect at your scan?
3
Growth scans are primarily transabdominal, although transvaginal imaging may be required to assess the placenta or cervical length. We assess baby’s growth, amniotic fluid, and blood flows at every appointment.
What is a placenta localisation scan?
1
A placenta localisation scan is performed to determine the exact position of your placenta in relation to the cervix (the opening of the uterus). If your placenta was noted to be low-lying at your morphology scan, a follow-up placenta localisation scan is usually recommended later in pregnancy to check whether the placenta has moved to a higher position as your uterus has grown.
Why is placenta position important?
2
The position of your placenta can affect your delivery plan. If the placenta remains close to or covering the cervix (known as placenta praevia), your doctor will discuss the safest options for your birth. In most cases, a placenta that appears low around 20 weeks will have moved clear of the cervix by the third trimester — more than 90% of low-positioned placentas identified in the second trimester resolve by the third trimester (Jansen et al., Ultrasound Obstet Gynecol 2020; see also RCOG Green-top Guideline No. 27a).
How to Prepare
• Timing: As per a fetal growth scan — this scan is a growth scan. Usually performed between 34 and 37 weeks, or as directed by your doctor
• Bladder: After 34 weeks, there is no bladder preparation required
• Appointment length: Approximately 20–30 minutes
• What to bring: Your referral letter, Medicare card, and your morphology or previous scan report
Will I need a transvaginal (internal) ultrasound?
3
In many cases, a transvaginal (internal) ultrasound is recommended as part of this assessment. The transvaginal approach provides a much clearer and more accurate view of the relationship between the lower edge of the placenta and the cervix compared with a transabdominal scan alone. As always, this is only ever performed with your consent, and your sonographer will explain why it is recommended before proceeding.
What is cervical length screening?
1
Cervical length screening uses transvaginal (internal) ultrasound to measure the length of your cervix during pregnancy. Transvaginal measurement is considered the reference standard for identifying a short cervix, which is associated with an increased risk of preterm birth. Your doctor may refer you for cervical length screening if you have a history of preterm delivery, cervical surgery, or other risk factors, or it may be assessed routinely as part of your morphology scan (ASA Clinical Practice Guideline: Ultrasound Assessment of the Gravid Cervix, 2023; ISUOG Practice Guidelines: role of ultrasound in the prediction of spontaneous preterm birth, Coutinho et al., Ultrasound Obstet Gynecol 2022).
What happens during the scan?
2
A slim, sterile transvaginal transducer is gently placed into the vagina to obtain an accurate measurement of the cervical length. This is a brief and generally well-tolerated procedure. Your sonographer will explain each step before and during the assessment. There is no threat to the pregnancy during a transvaginal scan.
How to Prepare
• Timing: Usually from 16 weeks onwards, as directed by your doctor
• Bladder: An empty bladder is required for cervical length measurement
• Appointment length: Approximately 15–30 minutes, and may be combined with a growth scan
• What to bring: Your referral letter and Medicare card
Ongoing Monitoring
3
If your cervical length is found to be shorter than expected, your doctor may recommend serial (repeated) measurements at regular intervals to monitor for any changes. These follow-up scans are short and focused, and your sonographer will ensure you are comfortable and informed at every visit.
What is 3D/4D Imaging?
1
3D and 4D ultrasound are advanced imaging techniques that allow you to see detailed, three-dimensional images of your baby. 3D imaging produces a still, lifelike image, while 4D adds the element of real-time movement — so you may see your baby yawning, stretching, or even smiling.
Our Expertise
2
At Central West Women’s Imaging, 3D/4D imaging is available for all women as part of our routine obstetric assessment. This is part of our commitment to providing the highest standard of obstetric ultrasound in regional New South Wales. Our sonographers are experienced experts in 3D/4D imaging techniques and use dedicated GE women’s imaging equipment optimised for this purpose.
While we are committed to giving you the best possible experience, we are unable to guarantee a particular 3D/4D image, as this depends on your baby’s position and the amount of fluid around them on the day. Our first priority is always a thorough, high-quality diagnostic ultrasound — we will do all we can within your appointment time to also capture 3D/4D images for you.
Please note: A current referral from your GP, obstetrician, or midwife is required for all ultrasound appointments.
What is different about a multiple pregnancy?
1
If you are expecting twins or triplets, your pregnancy will require more frequent ultrasound monitoring than a singleton pregnancy. The type and frequency of scans depend on whether your babies share a placenta (monochorionic) or each have their own (dichorionic), and whether they share an amniotic sac (ISUOG Practice Guidelines: role of ultrasound in twin pregnancy, Khalil et al., Ultrasound Obstet Gynecol 2025).
What are the types of twin pregnancy?
2
• Dichorionic diamniotic (DCDA): Each baby has their own placenta and amniotic sac. This is the most common type of twin pregnancy and is generally associated with fewer pregnancy complications than monochorionic types, although twin pregnancies of all types carry higher risks than singleton pregnancies (ISUOG 2025).
• Monochorionic diamniotic (MCDA): The babies share one placenta but have separate amniotic sacs. This type requires closer monitoring due to the shared placental circulation and the risk of conditions such as twin-to-twin transfusion syndrome (TTTS), twin anaemia-polycythaemia sequence (TAPS), and selective fetal growth restriction (ISUOG 2025).
• Monochorionic monoamniotic (MCMA): The babies share both a placenta and an amniotic sac. This is the least common type of twin pregnancy and requires the most frequent monitoring, including for the additional risk of cord entanglement (ISUOG 2025).
How to Prepare
• Timing: As directed by your doctor, with frequency depending on the type of multiple pregnancy
• Bladder: As per the specific scan type (see individual sections above)
• Appointment length: Allow additional time — typically 30–60 minutes depending on the scan type and number of babies
How often will I need scans?
3
Your doctor will advise a scan schedule tailored to your specific type of multiple pregnancy. As a general guide, and in line with international best practice, DCDA twins are typically assessed every four weeks from around 20–24 weeks, while MCDA twins are assessed every two weeks from 16 weeks due to the risk of shared placental complications. MCMA pregnancies require even more frequent assessment, often weekly, and usually in collaboration with a Maternal Fetal Medicine specialist. Each scan monitors the growth and wellbeing of each baby individually (ISUOG Practice Guidelines: role of ultrasound in twin pregnancy, Khalil et al., Ultrasound Obstet Gynecol 2025).
What to expect?
3
Scans for multiple pregnancies may take longer than singleton scans, as each baby is assessed individually. Your sonographer will measure each baby’s growth, check amniotic fluid levels around each baby, and assess blood flow where indicated. We understand that carrying multiples can bring additional questions and concerns — our team is here to support you and explain everything along the way.
Frequently Asked Questions
If you have any questions before your appointment, or would like to discuss any aspect of your scan, please do not hesitate to contact our friendly team.
-
Ultrasound is generally painless and safe for both you and your baby. The transabdominal scan feels like gentle pressure on your abdomen. The transvaginal (internal) scan may feel slightly unusual, but most women find it more comfortable than a Pap test. If you experience any discomfort, please let your sonographer know immediately.
-
Yes. Diagnostic ultrasound has been used in pregnancy care for decades and there are no known harmful effects to you or your baby. The sound waves used are at very low power levels and do not involve radiation of any kind.
-
Appointment times vary depending on the type of scan. As a general guide: dating scans and growth scans take 20–30 minutes, morphology scans take approximately 45 minutes, and cervical length checks take approximately 15–30 minutes (and may be combined with a growth scan). Scans for multiple pregnancies may take longer.
-
Yes. You will need a current referral from your GP, obstetrician, midwife, or fertility specialist to attend any ultrasound appointment. Please bring your referral with you on the day.
-
Sometimes your baby may be in a position that makes it difficult to obtain all the images and measurements needed. If this happens, your sonographer may ask you to move around gently, have a short walk, or come back for a brief follow-up scan. This is very common and nothing to worry about.
-
You are very welcome to bring someone with you — we encourage you to bring one adult to your appointment for support. As our ultrasound room has limited space, we kindly ask that where possible you avoid bringing children to your appointment. If you have any questions about this, please call 02 5343 1919 or email admin@cwwi.com.au ahead of your visit and our team will be happy to help.
-
If you would like to know the sex of your baby, please let your sonographer know at the beginning of your scan. We are usually able to determine this from the 16 weeks onwards, although it depends on your baby’s position on the day. If you prefer not to know, we will take care not to reveal this information.
-
Your detailed report and images are sent electronically to your referring doctor, usually within 24 to 48 hours. With your permission, we can also send you a link to images and short video clips from your scan that you can download and keep.
-
There is nothing special you need to do after your ultrasound — you can return to your normal activities straight away. There are no known side effects from diagnostic ultrasound.
-
Your reports and images are electronically sent to your referring doctor, giving them access to review the images themselves as needed. We use a dedicated women’s imaging reporting system and provide comprehensive reports prepared in collaboration with our specialist doctors.
With your permission, we can also send you a personal link to images and short video clips from your scan, which you can download and share with your family.
